Archive Note: This article was originally published on LinkedIn on July 12, 2025.
Reflecting from 2026: This remains one of the most personal things I have published. The alarm issue described here is still unresolved at the time of archiving, and I still feel just as strongly about it. If anyone from Insulet reads this, the offer to consult still stands.

If you've never lived with a chronic medical condition, it can be hard to grasp the impact of a truly life-changing medical device. I've recently been introduced to one such device: the Omnipod 5 by Insulet Corporation. This is a closed-loop insulin delivery system for diabetics like me. I've had type 1 diabetes since I was a kid, and in all that time I have never experienced such a genuinely game-changing method of treating it.
I feel people often play fast and loose with the expression "game-changer", so I try to reserve it for things that really deserve it. The Omnipod 5 deserves it. But game-changers are not always perfect, which is partly why I am writing this. Given the huge positives this device has brought into my life, I feel I owe it to give the full picture rather than just have a moan about the very significant but very fixable issues it still has. Insulet Corporation, you can make this closer to perfect with some small changes.
Before non-diabetics, or even newer diabetics, can really grasp how big a deal this is, it might help if I take you through my diabetes backstory. For me, all of this has been normal for decades. Thinking about it now, while writing this, has made me realise just how much things have changed. So let me rewind a bit and share an abridged version of my life with diabetes.
Growing Up in the Staccato Era

When I was diagnosed as a kid, treatment was blunt and mercilessly rigid. The standard approach back then was what you might call "staccato treatment". It consisted of two injections a day, lots of blood tests, and treating food as a prescribed fixture. The two injections were a fixed mixture of long-acting and short-acting insulin. The long-acting covered the whole day and the short-acting dealt with food. From memory, these injections were supposed to be taken at breakfast and with your evening meal, although I am a bit hazy on the specifics.
It sounds manageable on paper, doesn't it? Two injections: one for your background insulin needs (basal) and one to handle any carbs (bolus). The reality was anything but straightforward. I would describe this method as being similar to pouring an egg into your car radiator to seal a leak. Not perfect, but good enough to keep you going most of the time.
For me, it meant living on rails. Every meal had to be precisely planned or be a repeat of something with a known nutritional value. There was no real freedom to eat spontaneously or differently from one day to the next. Imagine being seven or eight years old, eating the same packed lunch every day at school because the only safe variable was which piece of fruit you might have, assuming it was not too sugary. Drinks? Always water to start with. Sugar-free options were practically non-existent back then. Absolutely forget sweets. In a few years' time, watch out for the new "diabetic" sweets. The expression "It's not so much that the bottom fell out of his world, but that the world fell out of his bottom" has real meaning to a diabetic trying diabetic sweets for the first time after years without any. Not pleasant.
So, this system led to a rather boring way of eating. You learned to treat food as medicine or fuel, and it was more of a gaffer tape solution for loosely replicating how the body naturally deals with carbohydrate. Not ideal, but not too bad most of the time. Your body, however, is not a machine and can catch you out when you stop concentrating.
The Nighttime Danger No One Saw

In the late 80s and 90s, tragically it was not uncommon for diabetics to pass away due to hypos. My parents tried to shield me from this by telling me a child from the same local clinic I attended had "moved away". It was more common than people might realise today. The older I got, the more I understood what had happened to those kids I'd seen in the waiting room, and that's when it all felt a little tougher to process. The old "staccato" approach left huge gaps for things to go terribly wrong, especially at night, which is when many of these kids "moved away".
The nighttime hypo was literally a killer. A hypo (or hypoglycaemic attack) is what happens when the insulin you give manually, because your pancreas has given up the ghost, is too much. It strips too much sugar from your blood and your body is essentially left without fuel to run properly. When you are awake, it is usually pretty easy to recognise this. You feel weaker, your vision goes blurry, thinking becomes harder, and if you are very low on sugar you can pass out. We have all seen marathon runners unable to stand as they approach the finish line. What you are seeing there is very much what a bad hypo can do. But as I said, during the day it is fine. It can be dealt with. As a diabetic kid on a strict diet, it was sometimes quite a good experience. Imagine being told to eat a Mars Bar or drink a Slush Puppy as medicine. When my insulin regime changed up a gear, I used this to my advantage quite a lot. But at night, how was this dealt with?
By luck. That is the honest answer. I lost count of how many times I crashed so hard overnight that I would wake up emerging from what I thought was a dream, having been jabbed by a horrendous injection (Glucagon), feeling very similar to that pre-vomit hangover state and then having to drink Lucozade and eat biscuits. I would often have a rather inflamed tongue as well, having been subconsciously trying to bite it off mid-seizure.
It is not overly dramatic to say that I owe a lot to my parents for getting me through that stage. They were the first "alarm system" available for me. They were the only safety net between me staying at home or "moving away".
MDI: The First Taste of Real Freedom

Around the age of twelve, my treatment shifted to Multiple Daily Injections (MDI) and for the first time I felt like I had some control.
MDI meant using "the pen", a new delivery device that let me inject short-acting insulin throughout the day on top of a single long-acting daily basal shot. For the first time, insulin could bend a little to fit my life instead of my life bending completely to fit the insulin.
This might sound trivial now, but back then it was revolutionary. It did not mean I could gorge on cake and sweets, but it did mean I could look at food with something resembling choice. Want an extra slice of toast? Inject for it. Fancy a slightly different lunch? You could adjust. It meant more injections, but by this point the only fear of needles I had was when they were in someone else's hand. It is strange how stabbing yourself feels normal, yet watching someone else do it to you is far harder to handle. I think it comes down to control. But as I said, for the freedom to eat almost what I wanted, I was happy to take more injections.
The key thing was that the two types of insulin were separated, and I could use this to play with my short-acting insulin and learn how it actually worked for me. Of course, being a kid, I learned to game the system too. I vividly remember figuring out how to "go low on purpose" before going to the cinema so I would need a bag of pic'n'mix as "medication". Risky? Probably. But when you are a teenager who has played by the rules for so long, you learn to grab freedom where you can.
The Early Tech Era: Blood Sugar Pole Balancing
But MDI was still largely guesswork. More variables opened up to you, and your fingers and injection sites became pincushions. I pricked my fingers dozens of times a day and sometimes injected just as much. The increased variables turned diabetes into more of a pole balancing act than ever. Sometimes you could get it right proactively, but often a day that started well with a proactive approach turned into a reactive day. Extra injections to deal with being high, then extra food to counteract giving too much insulin, then back to another injection. It could be a real pain in the backside.
Nighttimes did not immediately get much better with the move to MDI, but it did give me the chance to eventually figure out how to manage some of the issues I had overnight. I actually recall suggesting to my consultant when I was fifteen that giving my long-acting insulin just before bed was probably not the best idea. Since it was meant to last twenty-four hours, maybe it would be better to give it in the morning instead. Then I would be awake when it first started coming into action. That small change was key to massively reducing my nighttime hypos.
MDI was the treatment I used until quite recently. While not perfect, it allowed me to find a way to function as close to "normal" as possible. I have travelled the world, worked on every continent but Antarctica, and never felt like I was blocked from doing anything. Granted, it probably took a bit more thinking than most people would ever realise, but I could find a way of doing pretty much everything I wanted to try… apart from becoming a fighter pilot. Top Gun was my introduction to some of the hard limits that diabetes would impose.
The CGM: Saving My Fingers and Showing the Real Story
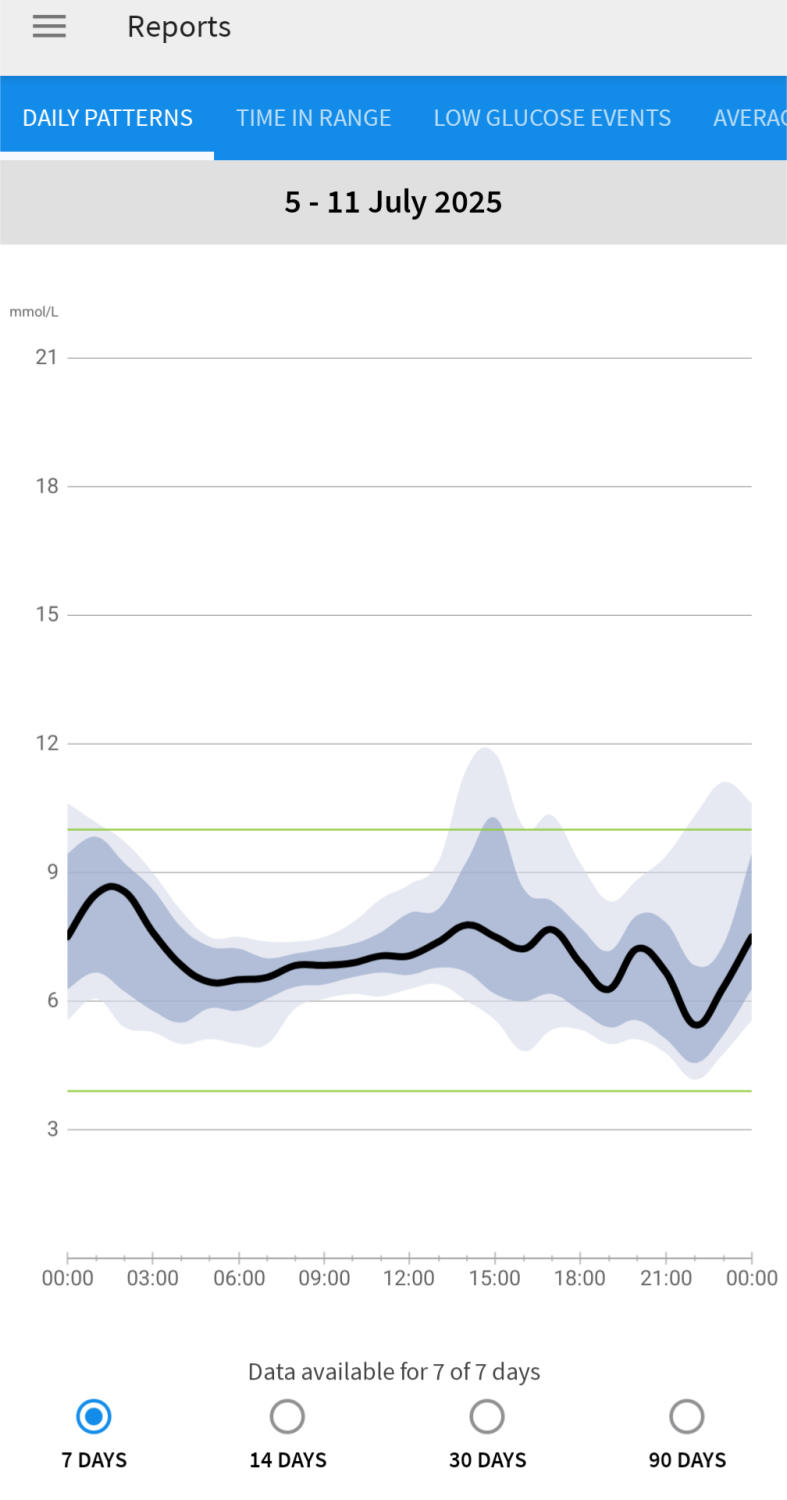
The introduction of continuous glucose monitors (CGMs) changed everything about how I monitored my diabetes a few years ago. Instead of piercing holes in my fingers a dozen times a day, I could wear a sensor instead. A tiny hair-thin filament sat under my skin and constantly read the glucose in my interstitial fluid, which is the fluid around your cells.
Multiple finger prick tests a day would only give me a result at a single point in time, but that did very little to paint a real picture of what was happening over the course of the day. I would generally test my blood to check what I thought were the extremes, highs or lows. So it was really just checking to see if my awareness of my blood sugar was accurate. But with a CGM, I could see the whole day mapped out in five-minute readings, even overnight. The other big improvement for diabetics using CGMs was the option to have alarms. You could choose to have an alarm go off if your blood sugar dropped to a dangerously low level. For me, that has never really been a need since I started using them, but for kids learning how their bodies work, it is priceless. There are also many people who have lost their hypo awareness entirely. I cannot imagine how tough it would be to not feel your blood sugar dropping while awake, but for people in that position, these alarms really are a game-changer.
The data the CGM gave me was genuinely interesting and helped me make a lot of improvements. I could spot daily patterns and adjust my injections to keep better control. It was fascinating to see how my body reacted when I went running or played tennis. You would think exercise would always bring your blood sugar down, and often it did, but sometimes my levels went up instead. Adrenaline released during sport can actually cause a diabetic to go high because the liver releases glucose from stored glycogen. The more you learn, the more you realise there are caveats to the rules you were given as a kid.
So I was finally in a position where I had better data, fewer finger pricks, and my body's blood sugar story laid out clearly in a graph. For a data nerd, this was addictive. But for all its power, the CGM did not deliver insulin. It gave me the information I needed to be better controlled, but it also led to more injections, because more data meant more adjustments for that constant pole balancing act. It made me better controlled, but it demanded a lot more interaction to make use of that data properly.
Why This Sets the Stage for a Real Revolution
Although this story has been long, it has all been leading towards one thing: better data enabling better results, but still only through manual pole balancing.
The CGM tells me what is happening inside my body every five minutes. But on its own, it still cannot act for me. It is like the old days of data integration, where you might have some of the latest systems ready to connect with everything around them but were still held back by the legacy system that could only import or export a CSV file once a day. Your new systems might have been designed to communicate in countless ways, but you were stuck with that legacy piece you just could not remove. An Enterprise Service Bus (ESB) would have solved that at the time, and in some ways the same thinking is what has moved diabetes treatment forward until the legacy system, my pancreas, can be replaced properly.
The missing piece has always been automation that actually works. A system that does not just show the data but acts on it in as close to real time as possible. That is what the Omnipod 5 has introduced. It is automation-assisted pole balancing.
How the Omnipod 5 Works: The Leap from Manual to Microdoses
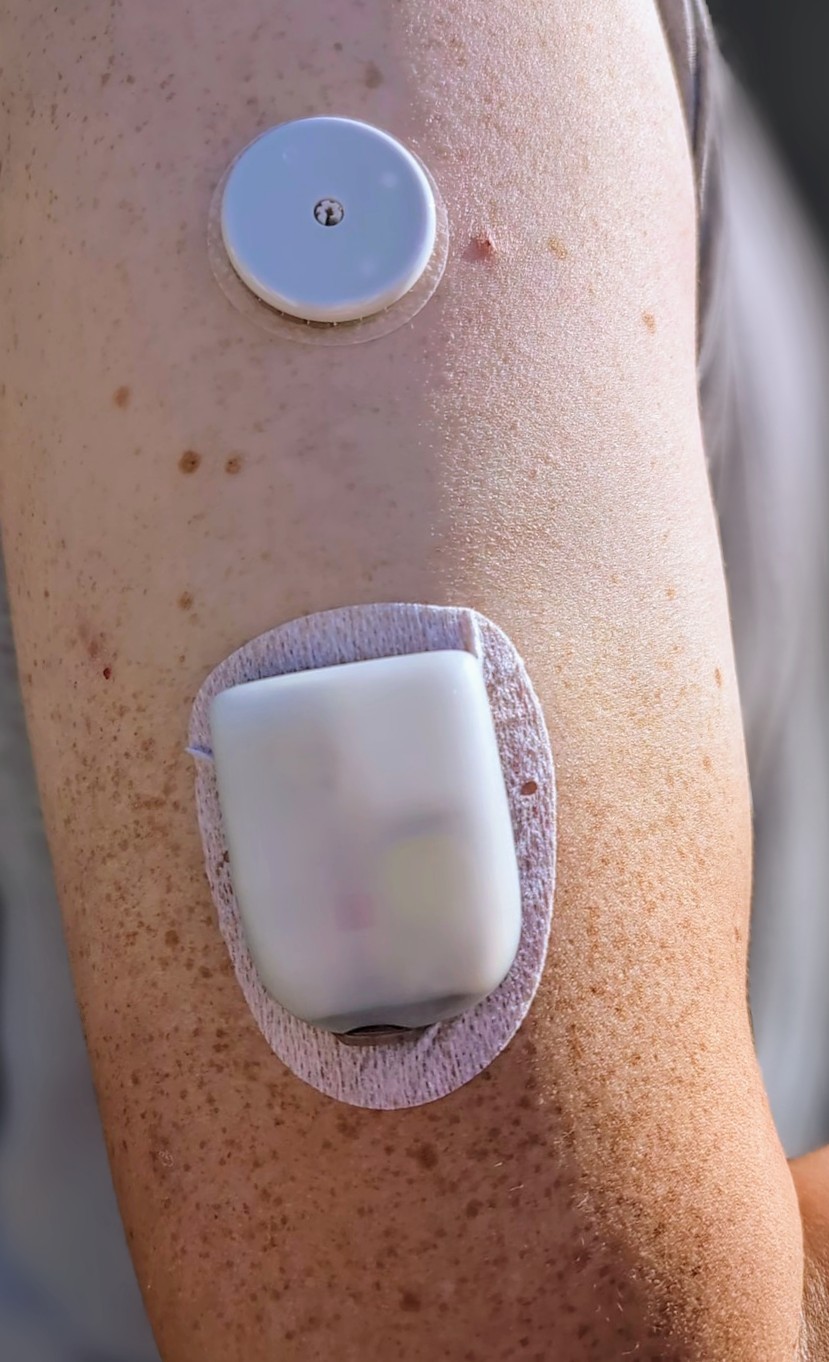
So what is the big leap in the right direction? For me, it is the closed-loop system. This means the Omnipod 5 talks directly to my Continuous Glucose Monitor (CGM), pulling my blood sugar reading every five minutes, around the clock. Since it is plugged in to me, it can immediately act on those readings. It gives microdoses of insulin every five minutes, or holds back if I am drifting too low.
Those tiny doses handle my basal insulin needs, which is the background insulin that keeps my body ticking over between meals. Instead of me guessing the right daily dose with one big shot that cannot be corrected afterwards, the Omnipod 5 adjusts it continuously.
Why does that matter? Because when your basal is managed by software, it effectively separates basal and bolus. That is huge. It means I can see my blood sugar changes for what they really are, or at least have a better chance of spotting the real cause. You would be amazed at how many things can make blood sugar rise or fall. But knowing your basal insulin is handled means you stand more of a chance of finding the true problem quickly.
Now when I eat, I just have to calculate the carbs, enter them into the Personal Diabetes Manager (PDM), and it works out my bolus dose based on the ratios I have set. I can even set different carb ratios for different times of day, because carb ratios are not fixed. In the morning my body needs fewer units of insulin per ten grams of carbohydrate than it does at lunch time, but more than it does in the evening. See how the original two-injections-a-day routine was so flawed?
I can also calculate correction doses of insulin if I am high on sugar for whatever reason. The correction factor needs to be calculated, but it is basically a measure of how much one unit of insulin will reduce your blood sugar level. I will be honest, this is not bulletproof and I strongly believe it should be adjustable by time of day, and possibly even by the current blood sugar level too. I have found that bringing blood sugar down can be a bit like stopping a moving train. When the train is moving slowly (a mild high), it only needs a gentle brake. When it is moving fast (a big spike), it needs a lot more force to stop. I do not think it is linear once you hit a certain point, and that is where I often disagree with the correction code. But it is a nice touch for novices. I tend to figure this out myself anyway. There is plenty of room for improvement here, Insulet Corporation.
Having this device control my basal insulin and make bolus control much easier has meant my blood sugar level has gone from sitting between 65 and 75 percent in range to between 85 and 95 percent in range. I still have bad days now and then, but I can handle those situations so much better than before.
Why the OmniPod 5 Is Truly a Game-Changer
1. Fewer Injections
- I worked out that I probably injected between 2,000 and 2,500 times a year when on the MDI system. While this did not bother me much (you get over injections pretty quickly when you start at age seven), it was an inconvenience and led to all sorts of complications you would not expect if you did not have to do it. Needing a spare needle when out at a mate's party in London at 1am is not an easy problem to solve.
2. Real-Time Basal Automation
- Microdoses every five minutes. Basal insulin is no longer a best guess. It is adjusted constantly, just like a healthy pancreas would do.
- Flat overnight lines. For the first time in decades, I can wake up with decent blood sugar levels almost guaranteed.
3. Separating Basal and Bolus: Data Clarity
- You can truly separate your fasting needs (basal) from your food needs (bolus). That means you can react more quickly to issues with blood sugar after food.
- Better pattern spotting. You get a clear idea of how different activities affect your carb to insulin ratios and how to work with that.
4. Reduces the Mental Load
- It does not remove the mental load, but it makes it significantly lighter. It allows you to redirect your thoughts onto more positive, solution-focused things.
- Diabetes is often described as having a second full-time job. This change has turned that into more of an intense time-consuming hobby, which feels far more manageable.
5. Fewer Surprise Highs and Gotcha Lows
- It does not completely stop the highs and lows, but it really does start to reduce them. These swings will always exist, but the OmniPod 5 makes them far easier to deal with.
6. Makes Living Normally Feel Possible
- It makes it easier to be spontaneous, with some caveats which I will explain in the next section.
- You can trust the system enough to take your brain off high alert for a few hours and just let it do its thing.
7. The Closest Thing Yet to a Real Artificial Pancreas
- Not perfect, but by far the best step so far.
- It gives you back some of the invisible "background processing" your pancreas used to do for free. I have forgotten what it is like to not have to think about insulin. But now I think about it a lot less.
The Flaw: When Safety Nets Become Shackles — And Cause Real Harm

The Omnipod 5 is a remarkable piece of tech. But here is the truth: a safety feature that does not trust its user can end up doing real damage, especially when that user has decades of experience managing a condition that was once far more dangerous than it is today.
I have lived through the years when alarms did not exist. As a kid, my parents were my alarm system. They dragged me back from nighttime hypos that really could have killed me, so I know exactly why alarms exist now. For people who cannot sense a low coming, they are literally lifesavers. But the problem with the Omnipod 5 is the blanket enforcement. It treats every diabetic the same, with forced, non-silenceable alarms, regardless of how well they know their own body.
Most people probably do not realise the real danger. Having used the Omnipod 5 for a while now, I can honestly say I would not have predicted this issue myself. So I do not blame Insulet for missing it, but I strongly urge them to take it into consideration. When you absolutely must stay silent, in places like theatres, the fear of that unexpected beep can push you into making bad decisions you would not otherwise make. A few weeks ago, I went to the theatre after having a meal out. I had guessed my dinner carbs pretty well, which is all you can really do when restaurants cannot tell you how many carbs are in a dish. I switched my PDM and phone off for the show, feeling confident enough to enjoy it. About fifteen minutes in, the pod alarm went off, loud enough for the people around me to hear. I could not check my sugar as my phone was switched off, but I did not feel low. Still, the alarm forced my hand. I ate some sweets to be on the safe side and, if I am honest, to shut the thing up before it went off again. But of course, it did go off again later, so I ate more. When I finally checked during the interval, I was not low at all. The alarm was simply telling me the pod would expire in a few hours. There is an eight-hour grace window anyway, so an alarm really isn't necessary, but I had no way to silence it, so I made a bad assumption and forced my sugar high just to avoid another alarm. Lesson learned, maybe, but what do I do if I go to the theatre again when my pod is close to expiry? Change it early and waste valid pod time just to be sure I will not start alarming at the wrong moment?
A similar thing happened at Wimbledon, this time three rows from the front on Court 1. These were fantastic seats. We'd worked for years to get seats this close using the ballot system and queuing. We'd finally got to a position where we could sit back, see everything and get a bit of sun as well. Unfortunately, I started going low on sugar, but I knew about it. Normally I would correct gently to avoid spiking high afterwards. But with no way to silence the alarm, and absolutely no desire to draw attention to myself while Ben Shelton was preparing to serve, I overcorrected. I stuffed in far more sugar than I would normally need just to guarantee the alarm would not go off. That meant hours of frustrating pole balancing afterwards, eating more, injecting more, trying to manage swings that would never have happened if I had simply been able to sit there quietly and let my blood sugar rise slowly.
I am bringing this up because it genuinely makes a positive piece of technology cause new problems. I have kept myself alive for nearly forty years with none of these safety mechanisms. I know what I am doing. I am not cross about the alarms existing, because for many they are a genuine safety net. But forcing them on everyone is the issue. A feature meant to protect me should not push me into making bad decisions simply to avoid embarrassment. I should be trusted to decide when I want that protection and when I do not. If that means signing a disclaimer, fine. I would probably not switch the alarms off most of the time, but at least I would have the assurance of knowing that they will not go off in moments when silence really matters.
I understand the legal side. Closed-loop insulin delivery must protect people. Too much insulin can kill you. But forcing the same rule on everyone is lazy design. It treats every experienced diabetic as if they are completely unaware of how to manage their condition. If Insulet Corporation want to make the Omnipod 5 as revolutionary as it deserves to be seen, they need to trust the people who have spent a lifetime learning how to trust themselves. That is how you build the next step in truly life-changing tech.
Source: This article was originally published on LinkedIn.
Status: Archived & Updated for rilhia.com.